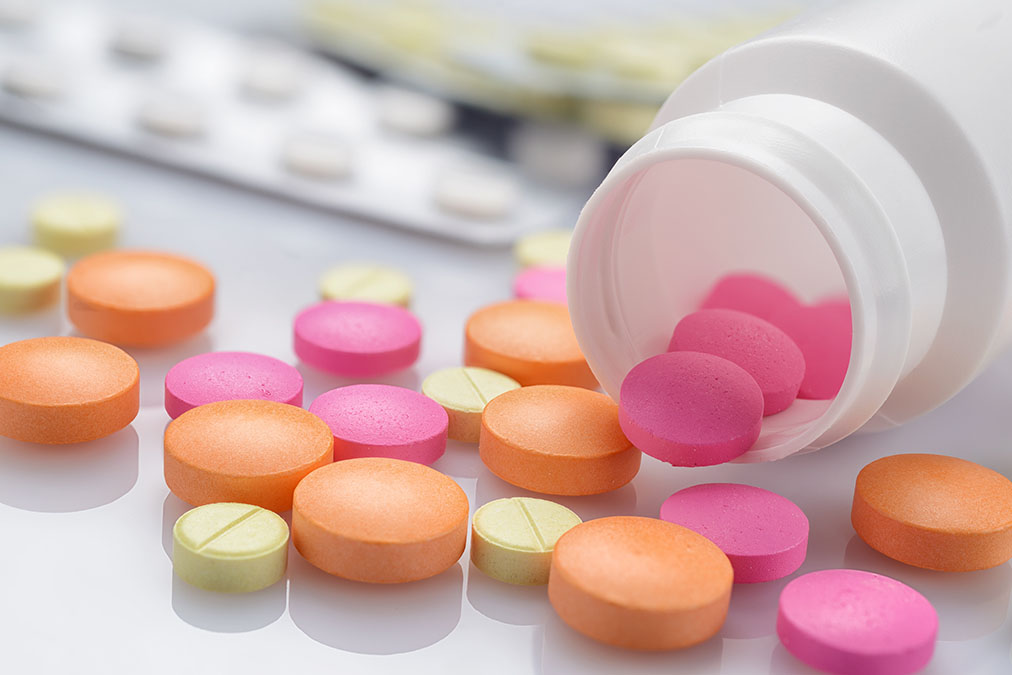
 Antibiotics have saved countless lives since Alexander Fleming first discovered penicillin in 1928.
Antibiotics have saved countless lives since Alexander Fleming first discovered penicillin in 1928.
But overuse has led to worries about bacteria becoming resistant to these commonly prescribed drugs.
That’s common knowledge of course, but what isn’t is the other potentially devastating health effects of their overuse. A new American study published in the European Heart Journal now suggests that too many courses of antibiotics are a red flag for greater heart attack risks.
Researchers analyzed the information of 36,429 women collected by the Nurse’s Health Study between 2004 and 2012. The participants were at least 60 years old in 2004 and they completed a health questionnaire every two years until 2012.
They were asked about their antibiotic use throughout their adult lives, between the ages of 20 and 39, between 40 and 59, and over 60 years of age.
They were divided into four groups based on their antibiotic use: those who had never taken any, those who had taken courses of 15 days or less, those who had taken courses of 15 to 60 days, and those who had taken courses longer than two months.
The scientists discovered that those who had taken antibiotics for two months or more when they were 60 and older had a 32 percent greater chance of developing cardiovascular disease compared to if they’d never taken any.
The women aged 40 to 59 who had taken at least one two-month course increased their risk of cardiovascular disease by 28 percent. Women below the age of 40 suffered no cardiovascular effects from these drugs.
It’s common when you hear about studies like this to wonder about other factors that might have affected the results, but the scientists were careful to account for smoking, diet, obesity, co-occurring health conditions, other medications, and so forth. In the end, they were sure that they were witnessing the effects of the antibiotics.
This is alarming if you’re older because you’re more likely to take antibiotics than younger people, but why should that be?
The authors offered two reasons to explain why antibiotics can have this effect.
Firstly, antibiotics destroy all bacteria, good and bad, which is bad news for the good bacteria in our intestines, the ones that help our bodies to fight off precisely those bacterial infections that then require us to take more antibiotics.
Secondly, good intestinal bacteria seem to have the ability to prevent inflammation, which is inextricably linked with cardiovascular disease. So, antibiotics deliver a double blow to older people.
The same authors presented a related study at the American Heart Association’s Epidemiology and Lifestyle conference in New Orleans in 2018.
From the same data, they found that women who had taken antibiotics from age 40 or over were 19 percent more likely to die of any disease later, and 57 percent were more likely to die of cardiovascular disease later when compared with their peers who had not taken any.

 Overcoming IBD
Overcoming IBD Multiple Sclerosis
Multiple Sclerosis Banishing Bronchitis
Banishing Bronchitis Gum Disease Gone
Gum Disease Gone Overcoming Onychomycosis
Overcoming Onychomycosis Neuropathy No More
Neuropathy No More The Prostate Protocol
The Prostate Protocol Brain Booster
Brain Booster
 Ironbound
Ironbound
 Solution for Shingles
Solution for Shingles
 The Bone Density Solution
The Bone Density Solution
 The Ultimate Healing Protocol
The Ultimate Healing Protocol
 The Parkinson's Protocol
The Parkinson's Protocol
 The Chronic Kidney Disease Solution
The Chronic Kidney Disease Solution
 Overthrowing Anxiety
Overthrowing Anxiety The Fatty Liver Solution
The Fatty Liver Solution The Hypothyroidism Solution
The Hypothyroidism Solution
 The End of Gout
The End of Gout The Blood Pressure Program
The Blood Pressure Program
 The Oxigized Cholesterol Strategy
The Oxigized Cholesterol Strategy
 Stop Snoring And Sleep Apnea Program
Stop Snoring And Sleep Apnea Program
 The Arthritis Strategy
The Arthritis Strategy The Vertigo & Dizziness Program
The Vertigo & Dizziness Program The 3-Step Diabetes Strategy
The 3-Step Diabetes Strategy Hemorrhoids Healing Protocol
Hemorrhoids Healing Protocol The Erectile Dysfunction Master
The Erectile Dysfunction Master Weight Loss Breeze
Weight Loss Breeze The IBS Program
The IBS Program The Insomnia Program
The Insomnia Program The Migraine and Headache Program
The Migraine and Headache Program The Neck Pain Solution
The Neck Pain Solution The Menopause Solution
The Menopause Solution The Ejaculation Master
The Ejaculation Master The TMJ Solution
The TMJ Solution The Acid Reflux Solution
The Acid Reflux Solution The Fibromyalgia Solution
The Fibromyalgia Solution The Psoriasis Strategy
The Psoriasis Strategy